
Starting July 5, Medicare is offering physicians a new payment model encouraging wearable devices – including smartwatches patients already own – to help track management of chronic conditions like high blood pressure, diabetes, musculoskeletal pain, and depression.
The Centers for Medicare & Medicaid Services (CMS) will run the voluntary Advancing Chronic Care with Effective, Scalable Solutions (ACCESS) Model for 10 years. It seeks to address chronic conditions CMS says affect more than two-thirds of Medicare patients:
- Early cardio-kidney-metabolic conditions (e.g., hypertension, dyslipidemia, obesity or overweight with marker of central obesity, and prediabetes),
- Cardio-kidney-metabolic conditions (e.g., diabetes, chronic kidney disease, or atherosclerotic cardiovascular disease),
- Chronic musculoskeletal pain, and
- Behavioral health.
The model encourages integrating Food and Drug Administration-authorized devices, such as those monitoring sleep, heart rate, and movement into a care plan that also may include lifestyle and behavioral support, patient education, and medication management.
ACCESS is open to patients with traditional Medicare who have at least one qualifying chronic condition included in one of the above clinical tracks. Patients can enroll directly with a physician or provider entity participating in the model or be referred by their physician. ACCESS-participating physicians can’t condition a patient’s enrollment on having the patient purchase, rent, or otherwise obtain a clinical device.
As with any program, proper due diligence – tailored to the physician’s practice – should be performed before signing up for ACCESS. The program’s payments are based on a fixed, recurring per-patient maximum where full payment is dependent on achieving a certain percentage of measurable health outcome targets. A physician should seek legal advice and understand how these payment parameters could affect their overall revenue.
Participating physicians will receive full payment if they achieve a given proportion of patients who meet measurable clinical standards determined by CMS, such as lowering systolic blood pressure and improving lab results for lipids and hemoglobin A1c.
“CMS will base payment on the overall share of an organization’s patients who meet their outcome targets, allowing organizations to earn full payment through strong overall performance even if some individual patients do not meet their target,” the agency explained on its website.
Per CMS, annual payment allowed amounts per patient will are divided into two categories: the initial period, or first 12 months of care, and the “follow-on” period, all subsequent 12-month periods. CMS notes the initial period payment “reflects the higher resource needs associated with onboarding, establishing care relationships, and achieving initial clinical improvement.”
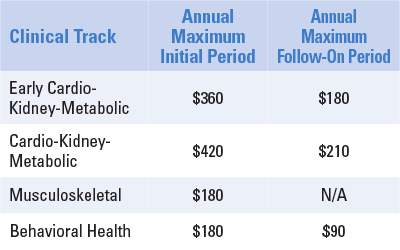
These allowed amounts represent the maximum annual payment per beneficiary for each track and include both the Medicare program payment (80%) and beneficiary coinsurance (20%).
CMS notes physicians participating in the ACCESS Model may wish to forego collection of beneficiary cost-sharing as a “beneficiary engagement incentive.”
Achieving the required percentage of health outcomes to receive the full allowed payment amount can hinge on factors physicians can’t fully control: whether patients consistently use their devices, take their medications, or are willing and able to make lifestyle changes, as well as nonclinical drivers such as access to food and housing or transportation challenges.
Tina Philip, DO, vice chair of the Texas Medical Association’s Council on Socioeconomics, notes devices can provide better monitoring for patients, pointing out she’s had patients report unusual heart rhythms like atrial fibrillation via heart rate monitoring on their smartwatches. But she also expresses concern that the model’s tracking and reporting requirements could – like other CMS programs – create more work for physicians.
“There’s a lot of value in some of this technology … but the level of reimbursement will need to match the work that goes into it,” the Round Rock family physician said.
Interested parties have until April 1 to apply via an online portal for consideration for the program’s first phase, beginning in July. Those applying after April 1 will be considered for program entry on Jan. 1, 2027.
While the FAQ section on the ACCESS website doesn’t make clear whether CMS provides funding for wearables, it does say:
- Participating physicians can provide wearables on a “loan or ownership basis” to patients;
- Participating physicians can order durable medical equipment such as continuous glucose monitors; and
- Patient-owned wearables (like smartwatches or fitness trackers) that align with ACCESS goals can be utilized on a voluntary “bring your own device” basis.
Physician groups must be actively enrolled in Medicare Part B to participate in ACCESS. More details are available in the ACCESS request for applications brochure. Primary care physicians and other clinicians not participating in the model can refer patients to ACCESS organizations and get regular electronic patient progress updates.
CMS notes while ACCESS is being testing in traditional Medicare, Medicare Advantage plans may independently adopt similar outcome-aligned payment arrangements with their contracted physicians and providers. Also, in February, CMS announced health plans that offer Medicare Advantage, Medicaid, and commercial insurance plans including Centene, Cigna, CVS Health, and UnitedHealthcare, “pledged to adopt an outcomes-based payment structure aligned to the Medicare-focused ACCESS Model.” Those could go live, per the pledge, as early as Jan. 1, 2028.
NOTICE: This information is provided as a commentary on legal issues and is not intended to provide advice on any specific legal matter. This information should NOT be considered legal advice and receipt of it does not create an attorney-client relationship. This is not a substitute for the advice of an attorney. The Office of the General Counsel of the Texas Medical Association provides this information with the express understanding that (1) no attorney-client relationship exists, (2) neither TMA nor its attorneys are engaged in providing legal advice, and (3) the information is of a general character. Although TMA has attempted to present materials that are accurate and useful, some material may be outdated, and TMA shall not be liable to anyone for any inaccuracy, error, or omission, regardless of cause, or for any damages resulting therefrom. You should not rely on this information when dealing with personal legal matters; rather legal advice from retained legal counsel should be sought. Any legal forms are only provided for the use of physicians in consultation with their attorneys. Certain links provided with this information connect to websites maintained by third parties. TMA has no control over these websites or the information, goods, or services provided by third parties. TMA shall have no liability for any use or reliance by a user on these third-party websites or the information provided therein.
Phil West
Associate Editor
(512) 370-1394
phil.west[at]texmed[dot]org

Phil West is a writer and editor whose publications include the Los Angeles Times, Seattle Times, Austin American-Statesman, and San Antonio Express-News. He earned a BA in journalism from the University of Washington and an MFA from the University of Texas at Austin’s James A. Michener Center for Writers. He lives in Austin with his wife, children, and a trio of free-spirited dogs.